Announcer: Welcome to ReachMD. You are listening to Advanced Treatments & Innovations from Mayo Clinic. For more information about Mayo Clinic, please visit mayoclinic.org
And, now here is your host.
Dr. Russell: Short for hyperthermic intraperitoneal chemotherapy, HIPEC is a unique procedure that’s used to treat stage 4 cancers that have spread inside the abdominal cavity, including cancers of the colon, ovary, and appendix. It can also be used to treat mesothelioma. But before we get too ahead of ourselves, today we’re going to be taking a look at some of the recent data on this novel treatment for advanced cancers. Welcome to Advanced Treatments and Innovations from Mayo Clinic on ReachMD. I’m Dr. John Russell and with me today is Dr. Nabil Wasif, a surgical oncologist from the Mayo Clinic. Dr. Wasif, thanks for being here today.
Dr. Wasif: It’s my pleasure. Thank you for having me.
Dr. Russell: So, before we dive into this topic, Dr. Wasif, can you give us some background on how cancers within the abdomen have traditionally been treated?
Dr. Wasif: Generally, they have been treated by what we call multimodality therapy. That is a combination of surgery, chemotherapy, and radiation. Out of these treatments, surgery is for what we call macroscopic disease, that is disease you can actually see with the naked eye, and radiation and chemotherapy typically for microscopic disease that is too small to be seen with the naked eye. The chemotherapy itself is usually given through the blood, or what we call systemically, and it reaches the tumor but also reaches other organs which accounts for the side effects, and the side effects really limit how much chemotherapy we can give our patients. In particular, for cancers that have spread within the abdomen, cure is rare, even when we combine all these therapies, primarily because it’s hard to get chemotherapy through the blood to reach those areas. This is not the case with HIPEC, which stands for hyperthermic intraoperative chemotherapy, which actually is a form of treatment for advanced cancers of the gastrointestinal tract. Currently, we’re using this for metastatic appendix, colon, ovarian cancers, and for peritoneal mesothelioma. We do recommend that a patient with any of these diseases should come and see us for a consult as soon as they are diagnosed with peritoneal carcinomatosis. Waiting too long has the problem that they – it may lead to further growth and then removal may just not be feasible. For many patients, we would also recommend that if they are on systemic chemotherapy and that has stopped working, they should be sent to us for a formal evaluation.
Dr. Russell: Thanks so much for providing that background, Dr. Wasif. And now that we have that reference point, what are some of the benefits and even some of the drawbacks of using HIPEC?
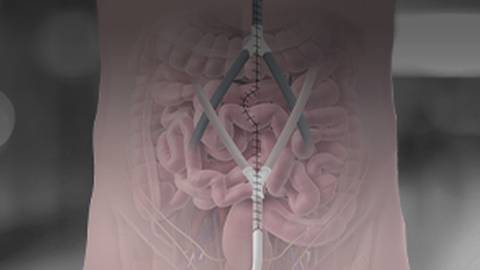
Dr. Wasif: I would say the main benefit of HIPEC is the actual possibility of cure for about 25% of patients with peritoneal metastases from the diseases I outlined previously. The goal still remains to remove all macroscopic, or visible, tumor with surgery, and then, using HIPEC during the surgery itself to eliminate the invisible, or microscopic tumor within the peritoneal cavity. Our theory is that if it’s not what you see that is the problem, it is the tumor cells that you don’t see at the time of surgery that may grow in the future to cause a recurrence. The way we give HIPEC is that it’s delivered directly into the abdomen following completion of surgery while the patient is still asleep. What that means is we can increase the dose of the chemotherapy by several orders of magnitude because we are putting it directly into the abdomen and not into the bloodstream, so we don’t have to worry about the side effects to that extent. It is also a one and done approach, which means that we are able to limit whatever toxicity may occur with the chemotherapy, such as hair loss, diarrhea, or mouth sores. Now, that is not to say that there are absolutely no side effects with HIPEC. We typically will put the chemotherapy in for about 90 minutes in the abdominal cavity and during this time, some of it, it’s still absorbed within the bloodstream. The main side effect that we do see are nausea, fatigue, a decrease in white cell counts, and, in rare cases, damage to the kidney. Luckily, all of these side effects are transient since the chemotherapy is out of the patient’s system in about 10 to 14 days. Given that surgery for these late stage cancers often involves moving multiple internal organs, the risk of surgical complications such as bleeding, infection, and death, is already higher than a typical surgical procedure. When you add chemotherapy to surgery, those risks increase. HIPEC usually is offered only to those individuals for whom other cancer treatment options are not available or already have proven unsuccessful, and who are healthy enough to withstand the rigors of such an aggressive treatment.
Dr. Russell: As I understand it, you’ve also done some research with your Mayo Clinic colleagues which looked at intermediate-term outcomes for patients. So, what did that study show?
Dr. Wasif: We presented findings from a retrospective study of intermediate-term outcomes for patients with peritoneal carcinomatosis treated with cytoreductive surgery and HIPEC. The study comprised 48 patients – 24 men and 24 women – who underwent cytoreductive surgery and HIPEC at Mayo Clinic’s campuses in Arizona and Florida from 2010 to 2014. The median age of the patients was 58, and 89% of the patients were white. The most common indication in our study was mucinous adenocarcinoma of the appendix – about 56% - and the second most common was metastasis from colorectal adenocarcinoma – about 31%. The majority of these tumors were low-grade – about 60% – and systemic therapy was given to about 46% of patients prior to cytoreductive surgery and HIPEC. The majority of these operations were performed with curative intent – about 80% of the time, we went in trying to actually cure these patients. Our results showed that we were able to completely remove all the tumor in 65% of patients. There was no 30-day postoperative mortality; however, 60% of patients did have some kind of a postoperative complication. Of these, 34% were serious complications, or what we call grade 4. With the median follow-up of 12 months, 48% of patients had no evidence of disease and 29% are still alive with disease. For all patients, the median recurrence-free survival, defined as being alive with no evidence of disease, was 19 months and 19% at two years. In the subset of patients who underwent surgery with curative intent, the median recurrence-free survival was 23 months and 25% at two years.
Dr. Russell: For those just tuning in, you’re listening to Advanced Treatments and Innovations from Mayo Clinic on ReachMD. I’m Dr. John Russell and here with me today is Dr. Nabil Wasif, who’s sharing results from a Mayo Clinic study that followed patients who were treated with hyperthermic intraperitoneal chemotherapy, or HIPEC. So, Dr. Wasif, earlier you explained that based on that study, patients who received HIPEC saw improved survival rates. Are there any other notable studies by your group on the topic?
Dr. Wasif: Our most recent publication on the topic looked at how our length of stay and complication rates changed after implementation of an enhanced recovery after surgery, or ERAS program. ERAS principles are related to moving away from traditional postoperative management that involves high-dose narcotics for pain control and lots of intravenous fluid and not feeding patients early. A major impediment to the use of HIPEC – and we saw this in our prior study – is the traditionally high rates of complications and the prolonged duration of time that patients would need to spend in the hospital. So, this study was really geared towards addressing this Achille’s heel of HIPEC. In our study of 130 patients, our total mortality was 0.8%, and we saw a reduction in major complication rates from 24% to 15%. We were also able to decrease our mean length of stay following surgery from 10 to 7 days. These are some of the best outcomes reported in the literature for HIPEC and are comparable now to the morbidity and mortality following any other major surgery. We think that our study should help allay some of the concerns about the excessive complication rates following HIPEC.
Dr. Russell: And doctor, knowing what you do now from the ongoing results of your studies, has your approach to cancer care changed at all?
Dr. Wasif: Absolutely it has. We do know that the complication rate can adversely affect our patients. Our work with Enhanced Recovery Pathways has enabled us to improve this aspect of HIPEC so that we can offer this service to more patients. The next step is to move on to the efficacy of the procedure itself. We know that for certain types of advanced peritoneal tumors, HIPEC is the most effective treatment. Prior to HIPEC, almost no one survived these diseases. For mesothelioma, the long-term survival rate is now about 50%, and for appendiceal cancer, about 60% at 10 years. The survival rates for ovarian and colon cancer are not as good, but this is something that we will continue to work on for the future.
Dr. Russell: Dr. Wasif, unfortunately, we’re almost out of time. But my last question to you before we wrap up is what do you want to make sure clinicians take away from this research and our discussion around it?
Dr. Wasif: I think I would summarize the state of the art for HIPEC as saying that is now standard of care for metastatic appendiceal cancer and peritoneal mesothelioma in the United States. In Europe, HIPEC is also accepted as standard of care for metastatic colon cancer; however, that is not the case in the United States yet. We did try to do a randomized trial on the subject, but it failed to accrue and was closed. However, even in the United States, many centers, including ours, continue to offer HIPEC for metastatic colon cancer. The latest application is for advanced ovarian cancer, and patients with this disease should also be referred to a HIPEC center. I will add that not everyone is eligible for HIPEC. Generally, a patient who has visceral metastases, such as liver, would not be a good candidate. However, if you think you have a patient who may benefit, then referral to a HIPEC Center of Excellence is strongly suggested. I think our biggest contribution has been to reduce the complication rate associated with HIPEC by implementation of an enhanced recovery after-surgery program. We have become more aggressive with how we treat these advanced cancers, but our focus on improving quality of life is really what gives me hope that more patients will be able to benefit. At Mayo Clinic, we want to work with our referring provider colleagues to help diagnose and treat our patients together. We want the best outcome for all patients, and we hope to continue to push for and find the best solutions.
Dr. Russell: Well, with those great takeaways in mind, I want to thank my guest, Dr. Nabil Wasif, for helping us better understand some of the latest investigations and treatment options surrounding HIPEC. Dr. Wasif, it was great speaking with you today.
Dr. Wasif: Thank you, very much, for having me. It was a pleasure.
Announcer: You’ve been listening to ReachMD. The preceding episode was brought to you by Mayo Clinic. To download this podcast and others in this series visit reachmd.com/mayoclinicinnovations. Thank you for listening.